Polyhydramnios Overview
Polyhydramnios is a pregnancy complication involving too much amniotic fluid that requires careful monitoring during the third trimester.
For many moms, learning they have too much amniotic fluid is scary, and overwhelming… especially learning about the risks. And then a healthcare provider says the words, “something wrong with your baby” and time stands still.
We understand because we’ve been there too.
We began our polyhydramnios journeys pretty much the same way: sometime during the second half of our pregnancy, hearing the words “too much amniotic fluid” or “polyhydramnios of pregnancy,” followed by the same paralyzing fear that our babies weren’t safe. Then our anxiety was fueled further by the same scary information most other poly moms find, courtesy of Dr. Google.
At KP, we do share the scary facts, but our main goal is to HELP you.
- To help you be the best advocate for your baby and yourself
- To help you separate the facts from the fluff
- To help connect you to a community of other poly mamas
- To help you through your fears and anxieties
- To help support you in any way that we can
- To do the research needed to pave the way for change
- To give every baby affected by a Polyhydramnios pregnancy the opportunity to thrive to their fullest potential.
This page contains an in-depth overview of everything you need to know about Polyhydramnios in pregnancy. It is intended to help women affected by Polyhydramnios to navigate the rest of their third trimester in safety and peace of mind.
Make sure to click on the links to the other pages on our site. They are filled with valuable, helpful information, all of which is backed up by either medical research or experience from other women affected by Polyhydramnios.
Table of Contents
Overview
What is Polyhydramnios?
Polyhydramnios is a rare pregnancy condition in which too much amniotic fluid accumulates around the baby inside the uterus. It generally appears in the third trimester, affects 1-2% of all pregnancies, and is associated with a high risk of poor pregnancy outcomes.
Polyhydramnios cases range from mild to severe. Management of the condition is highly dependent on the cause and the severity. Mild cases may be identified as idiopathic (meaning there is no known cause) and sometimes clear up on their own. While moderate and severe cases are more likely to be linked to maternal or fetal anomalies and may require closer monitoring and further testing.
What is Amniotic Fluid Index (AFI)
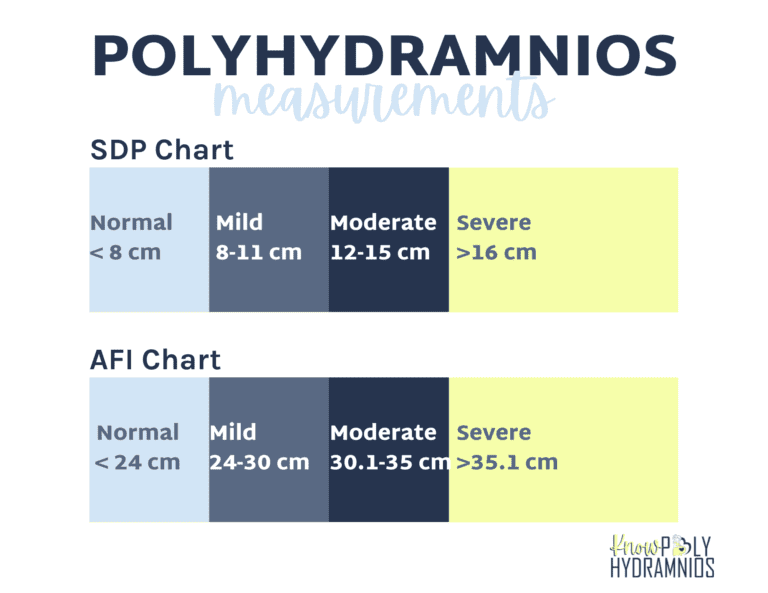
Polyhydramnios is most often diagnosed based off of the measurement of amniotic fluid. The most common ways to measure amniotic fluid are using the Single Deepest Pocket (SDP) or the Amniotic Fluid Index (AFI).
To get these measurements, the belly is divided into four quadrants and the deepest vertical pocket of fluid is measured in centimeters by ultrasound in each pocket. SDP is the measurement of one deepest pocket of fluid and AFI is the measurement of all four pockets added together.
Polyhydramnios is classified as mild, moderate, or severe based on the level of fluid found. However, the measurement of amniotic fluid is highly subjective, and current guidelines do not account for the fact that amniotic fluid naturally decreases during the third trimester.
KP offers FREE Fluid Trackers to gauge where a woman’s fluid level is compared to where it is expected to be. Fluid Trackers are available in our Member Area.
Then download and print your own fluid trackers from our member area.
Symptoms of Polyhydramnios
Polyhydramnios can cause:
- Breathing difficulties
- Swelling in the lower extremities
- Swelling of the vulva
- Constipation
- Increased heartburn/indigestion
- Tightness in the abdominal wall
- Increased contractions/Braxton hicks
- Fetal malposition (breech baby)
- Enlarged uterus/measuring ahead
Read more about the symptoms of Polyhydramnios plus tips for managing them.
Causes of Polyhydramnios
There is not always a clear cause for Polyhydramnios, which is why as many as 60% of cases are considered idiopathic at the time of delivery. Idiopathic does NOT mean there is no cause, instead, it means that the cause has not been identified yet.
Studies have shown that only 17% of mild cases are caused by an underlying disease. On the other hand, 91% of moderate/severe cases of Polyhydramnios are linked to an underlying disease.
In cases where the reason is known, Polyhydramnios is usually linked to problems causing reduced fetal swallowing or increased fetal urination. Although it has also been known to be caused by fetal heart conditions and problems with the placenta.
Read our comprehensive list of known causes of Polyhydramnios here.
Risks Associated with Polyhydramnios
Polyhydramnios may increase the risk of these problems:
- Preterm labor
- Premature rupture of membranes (PROM)
- Preterm Premature Rupture of Membranes (PPROM)
- Preeclampsia
- Fetal Malpresentation
- Umbilical cord prolapse (UCP)
- Placental abruption
- Emergency or Unplanned C-section
- Stillbirth
- Postpartum hemorrhage
- Macrosomia
- Pulmonary Embolism
- Amniotic Fluid Embolism
What Follow-up Tests do I Need with Polyhydramnios?
Standard tests all women need:
- Oral glucose tolerance test (GTT)
- Non-stress test (NST)
- Biophysical Profile (BPP)
- Growth scan
Additional screening tests may include:
- Fetal echocardiogram
- Maternal blood grouping and rhesus factor antibody screening
- Maternal ToRCH screening
- Middle Cerebral Artery (MCA) peak systolic velocity test
- Karyotyping/Microarray
- Whole Exome Sequencing (WES)
Treatment for Polyhydramnios
Treatment for Polyhydramnios depends on the cause and the severity of each individual case. It usually involves the effective management of known conditions.
Mild, idiopathic cases may not require any special treatment, but should still be monitored for potential changes. Fetal surveillance is recommended every other week until 37 weeks, then weekly until delivery.
Moderate/severe idiopathic cases need closer monitoring of both mother and baby. Fetal surveillance is recommended weekly either until Polyhydramnios resolves or until delivery.
Polyhydramnios complicated by other high-risk factors such as the early onset of severe Polyhydramnios, Polyhydramnios complicated by IUGR, or Polyhydramnios accompanied by known fetal anomalies should be considered very concerning. These cases require twice-weekly fetal surveillance, referral to genetics and a maternal-fetal medicine specialist, and possible interventions like amnioreduction.
Cases caused by certain underlying diseases, such as diabetes or fetal heart problems, require effective management of the underlying disease and close monitoring of both mother and baby.
In cases where the underlying condition cannot be managed prenatally, very close monitoring and delivery interventions may be needed. This also applies to cases of moderate/severe idiopathic Polyhydramnios.
How Common is Polyhydramnios?
- 1% of pregnancies are complicated by Polyhydramnios
- 65% of these cases are mild
- 20% are moderate
- 15% are severe
- The average OB in America only sees ONE case of polyhydramnios each year
- 61% of cases are considered idiopathic at the time of delivery
- 18% are caused by a genetic anomaly
- 10% are attributed to a blood incompatibility or infection
- 4% are caused by fetal anemia
- 4% are due to complications of twin pregnancy
- 3% are caused by Gestational Diabetes
- 1/3 of idiopathic cases will find the cause before the baby’s first birthday
You can find these and many more statistics related to Polyhydramnios by clicking right here.
How to Reduce Amniotic Fluid
In some cases, a diabetic diet has helped to reduce and control amniotic fluid levels. This has been especially true for moms with diabetes, or high fasting blood sugars. Other moms have claimed that they saw reduced fluid levels after using tissue salts and Nat Mur. At this time, there is no clinical evidence to support any of these claims though, so women wishing to try these options should consult their healthcare team before trying any of these methods.
In cases of very severe amniotic fluid levels, amnioreduction can be used to temporarily reduce fluid levels in order to prolong a pregnancy at risk of preterm delivery.
Indomethacin is a medication usually given to stop preterm labor during the second trimester. One of the effects of indomethacin is to reduce amniotic fluid levels. Even though it does temporarily reduce fluid levels, the SMFM does NOT RECOMMEND the use of indomethacin for the sole purpose of reducing fluid due to the risks of heart complications to the unborn baby.
Read more about the methods used to reduce amniotic fluid here.
Does Reducing Amniotic Fluid Even Help?
The biggest danger in having too much fluid lies in the risks it creates, especially for placental abruption. So, it makes sense that the more fluid a woman carries, the higher her risk, and that lowering that fluid can help reduce the risk. Lowering fluid levels can sometimes help to reduce the risks of Polyhydramnios, especially during labor and delivery.
However, reducing amniotic fluid does not take away what caused it to be high in the first place. It’s very important to remember that Polyhydramnios is a secondary condition. It is the result of something else (even idiopathic cases because there is still a cause, it’s just not known). So, even if a woman has managed to lower her fluid level and avoided serious complications during labor and delivery, her baby may still have an underlying health condition that needs to be addressed.
Labor & Delivery with Polyhydramnios
Mild/Moderate Idiopathic Polyhydramnios with no other fetal or maternal complications: full-term delivery between 40+0 and 40+6 weeks gestation in a perinatal center is recommended.
Mild/Moderate Polyhydramnios with fetal, maternal, or other obstetric complications: the timing of delivery for the indicated condition should take precedence. Delivery in these instances may need to take place in a tertiary center with access to specialty care.
Severe Idiopathic Polyhydramnios: delivery between 38+0 and 38+6 weeks at a tertiary center with access to specialty care is recommended.
Severe Polyhydramnios with known fetal anomalies, early onset of severe Polyhydramnios, or Polyhydramnios accompanied by fetal growth restriction: delivery at 37 weeks at a tertiary center with access to specialty care is recommended.
You may also like our resource about balloon catheter inductions with polyhydramnios. There is mounting evidence that has led us to believe that balloon catheters are NOT SAFE and SHOULD NOT BE USED in mothers with Polyhydramnios.
What Questions Should I Ask My Doctor About Polyhydramnios?
Many women diagnosed with Polyhydramnios have a long list of questions for their health care providers. We’ve compiled a very thorough 3-page printable questionnaire for women who find themselves at a loss for what to ask.
Not every question may apply to every situation, and certain women may need to add questions. That’s totally okay! Click here to go to our “questions for your doctor” page and preview the list. You can also download and print a copy from our member area.
Postpartum Signs to Watch out for after Polyhydramnios in Pregnancy
Having Polyhydramnios during pregnancy puts a woman at a higher risk of postpartum hemorrhage, pulmonary embolism, and amniotic fluid embolism. All of these conditions can be life-threatening and are considered emergency situations.
After delivery, mothers will be monitored closely for signs of uterine atony, when the uterus remains soft and doesn’t contract. If the uterus doesn’t contract, the blood vessels that were attached to the placenta don’t get compressed and then bleed freely. This can lead to postpartum hemorrhage (uncontrolled bleeding).
Mothers should also be monitored for signs of a blood clot or deep vein thrombosis (DVT) in their arms and legs. A DVT can break free and block the arteries in a woman’s lungs which quickly becomes a life threatening emergency known as Pulmonary Embolism (PE). PE is one of the leading causes of maternal mortality around the world.
Amniotic Fluid Embolism is an extremely rare, but extremely deadly complication where amniotic fluid enters the maternal blood stream, causing a life threatening allergic-type reaction. (It’s important to note here that not everyone has this type of reaction. Sometimes amniotic fluid or fetal tissue enters the maternal bloodstream and there is no reaction at all. The danger is that there’s no way to tell who will have a reaction and who won’t.) Symptoms of Amniotic Fluid Embolism usually begin shortly after birth. If a mother is having trouble breathing or experiencing chest pain, her health care team needs to be alerted right away.
Will My Baby be Okay if I have Polyhydramnios?
Pediatric support should be made available to every baby affected by a Polyhydramnios pregnancy, even if there has not been an antenatal diagnosis of a genetic anomaly. The risk of finding a previously undiagnosed anomaly in these babies is 9% during the immediate neonatal –period, and as high as 28% up to one year later.
It is recommended by the NHS that an NG tube be passed before the baby’s first feeding to rule out blockages that could have been missed via ultrasound during pregnancy. Esophageal atresia and tracheoesophageal fistula are the most commonly missed anomalies on fetal ultrasound, so passing an NG tube helps to rule these problems out.
All babies will be evaluated shortly after birth. Low 1 minute APGAR scores are common in Polyhydramnios babies, but usually improve by 5 minutes. Women should be prepared for the possibility that their baby may need breathing assistance since many Polyhydramnios babies show signs of respiratory distress. This is also the reason that Polyhydramnios babies are associated with a higher rate of NICU admittance than the general population.
If a woman’s Polyhydramnios was caused by a known fetal anomaly, her care team should have a plan in place that may involve her baby being taken immediately into surgery or straight to the NICU.
We can’t say for certain that every baby will be okay or not. But what we can do is offer support and accurate information that can help women to help their babies. If you haven’t already found a Polyhydramnios Support group this list is a great place to start.
FAQs
FAQs
Polyhydramnios has been associated with increased weight gain. The increase in fluid, combined with a larger than average baby in some cases can lead to extra weight gain during pregnancy.
Being diagnosed with Polyhydramnios can be very worrisome for a lot of women. But knowledge is power! Understanding the risks involved and creating a carefully laid out plan for the management of your pregnancy, labor, delivery, and postpartum can help you to feel more in control. You can also join a support group to help you through this difficult time. Check out our list of support groups right here, and download a printable list of questions for your doctor here.
References for Further Reading
All of our recommendations are evidence based, compiled from medical journals, research studies, hospital guidelines, and other obstetrics/gynecological/midwifery publications such as:
Read Next
AFI (Amniotic Fluid Index) – Amniotic Fluid Index, AFI, is the sum total measurement of the deepest pocket of amniotic fluid in each of the four quadrants of your uterus.