
Jackilyn's Story: Victory of an Immovable Voice
- Jackilyn's Story
- Updates

Victory of an Immovable Voice
Jackilyn’s story is an empowering example of how to advocate for the care you need. If she hadn’t she wouldn’t be alive today, and neither would her baby. Jackilyn’s incredible story of survival will inspire you to do your own research, trust your instincts, and be the very best advocate for yourself.
I watched two stories, in particular, unfold during my poly pregnancy that fueled my passion to want to create this website. Jackilyn’s story was one of them. I am so grateful that she wanted to tell her story here to help empower other mamas during such an anxiety-filled time.
Thank you, Jackilyn, for telling your story!
Trigger Warning
Jackilyn’s story mentions PPROM, premature labor, emergency c-section, NICU time, multiple infections, postpartum hemorrhage, emergency exploratory surgery, blood transfusions, fetal anemia, and a near-death experience. I encourage you to read it though and make it all the way to the end. Jackilyn has an uncanny ability to advocate for herself. That drive saved her life, saved her preemie warrior, and I know it will inspire you too.
When I was around 15 years old I saw the film Jersey Girl. When I saw Jennifer Lopez die during childbirth, I got this dreadful feeling in my stomach. Call it a warning, women’s intuition, manifestation, or paranoia, but I knew if I ever gave birth something terrible would happen to me. As the founder of my city would say, “Whether you think you can or you think you can’t either way you are usually right.”
I became pregnant just a week prior to Thanksgiving 2019 and besides nausea 24/7 and a weird rash, all was normal. Then my 20-week ultrasound revealed I had placenta previa but would likely correct itself. I was very anxious but on May 22nd I had a scan that confirmed it was corrected and I was thrilled! However, being a heart ultrasound tech myself, I recognized the tech’s face that something was wrong. I was by myself because of covid. I was measuring at 40 weeks at 28 weeks. I had been very uncomfortable and swollen but all dismissed my concerns as a normal pregnancy. She went and talked to the doctor, but told me I needed to follow up with my doctor because I had moderate polyhydramnios which wasn’t there on the prior ultrasound. My AFI was 32, no diabetes, or reasons for the fluid aka idiopathic. This confirmed my suspicion something terrible was going to happen to me, but everyone encouraged all would be fine.
For a few weeks, I had been “leaking” which I was told on the phone was likely urine due to extra pressure on my belly. I had an extra liter of amniotic fluid in there after all! However, after the diagnosis, I insisted I be seen in the office for my RH shot as it is the incompatibility cause for poly. I researched poly all weekend prior to my visit. I got the shot, and also was told I was likely leaking amniotic fluid and we were not to worry as I had a lot. I insisted I get set up with an MFM appointment and have a weekly NST. On June 3rd my NST was normal aka nonreactive. Nonetheless, immediately afterward I went to the bathroom and lost my mucus plug! My doctor told me to monitor for contractions and continue normally no bed rest needed. I made an appointment with the MFM for June 8th.
Five days later on June 8th, I woke up at midnight to urinate like I did every night. However, at 3 a.m. I awoke to a warm GUSH all over my pregnancy pillow, sheets, and mattress. I yelled to my husband my water broke and leaked on our hardwood floor and carpet all the way to the bathroom. I thankfully had just packed my hospital bag two days prior! I got on my hands and knees to prevent cord prolapse and my husband called the ambulance. Our on-call doctor wasn’t responding. I quickly learned the EMTs couldn’t take us to the hospital we wanted. So, I demanded they pull over and we parked in a parking lot across from the hospital until my husband arrived about 10 minutes later. My contractions hadn’t started and I was stable. I signed paperwork, and my husband drove us when my contractions started. I called ahead for PPROM and was taken to triage. Still no answer from the OB.
In triage, I was tested for Covid, and magnesium was started to try and stop the labor and for fetal neuroprotection, as well as steroid shot for lung development, and antibiotics with gestational HTN. I was told I’d be monitored in antepartum for a minimum of 3 weeks as I was only 31 weeks and they wanted me to get to 34. Because of the full moon, however, they were full so we went to labor and delivery to wait for a room. My placenta was anterior but my continuous NST monitor was good and all my fluid was gone, and the mag successfully stopped my labor. We were transferred late to antepartum-which I knew was a covid unit as I worked in the hospital and was scared so I asked to be transferred but they didn’t have room. They said visiting hours were over and at 10 pm tried to make my husband go home. I got the charge and insisted he stay as he hadn’t slept and I was just admitted. She and our new RN agreed to take responsibility. I cried all night about being alone for 3 weeks to be monitored in the tiny room.
The next morning on June 9th my OB said I was free to go take a walk and told my husband he could go home. However, they scheduled an ultrasound at 11 am to check baby’s growth so wanted to wait until after as due to covid he had only seen her on ultrasound 1/5 ultrasounds. It was a good thing because around 10 am I knew something was wrong and I pushed my nurse to get the NST monitor. At 10:45 my contractions had increased in intensity and timing and nobody came to get me for the ultrasound. Instead, the resident and nurses came in as baby’s HR spiked to 170s and I rapidly developed a fever of 101 and was rushed to L&D. I was diagnosed with an infection called chorioamnionitis, an infection of the amniotic fluid, that may have caused my water to break as it can take time to show despite antibiotics. My other OB came in at noon and I was quickly prepped for an emergency C-section as I didn’t dilate and it was life-threatening to us both. The infection made the contractions worse and my fever was dreadful. I also had mag restarted which we know mag is a drag. I got a spinal IV with morphine and fentanyl and antibiotics. Aerilyn Kate was removed at 1:09 weighing 2 lbs 14 oz and was taken to the NICU after they resuscitated her. We couldn’t hold her. My husband followed her to the NICU while I got stitched up and stayed in recovery for standard two hours.
In recovery, I was alone until my Doula fought her way through the hospital doors. With covid, she wasn’t allowed and neither were any visitors. I was very emotional and overwhelmed with guilt and my nurse took us to see her in the NICU before going to our room. My little girl was placed on Cpap and got calcium and phosphorus as her bones were not developed. She couldn’t eat until 34 weeks and was on an ng tube, had a blood transfusion for anemia and antibiotics. We were told I’d be there a few days but recovered very well and was able to walk to the bathroom, cough, and lift my legs! I was dehydrated and nauseous so I couldn’t eat as they upped my saline. I went to finally do skin-to-skin with my daughter in the NICU, but they made me go back upstairs because I was falling asleep.
On June 10th around 5 am I had abdominal pain after my C-section and I was still very swollen from all the fluids and previous poly edema. I had shoulder pain and low urine output. They kept telling me I just had major surgery, but I pushed for my older nurse to get the chief resident who we trusted and assisted in my surgery and diagnosed my infection. My stomach was distended and I was scheduled to get a STAT CT at 10 am in meantime drew a CBC. My hemoglobin dropped from 12 to 6 so ultrasound DIVA was called because of the swelling to get a new IV to start a blood transfusion. It took a while to order the blood and for the DIVA to come, so I asked him to draw my blood again as my husband said I was pale and couldn’t stay awake. It came back as a critical level of 3.9! If not for our insistence of a repeat blood draw I would have died from the hemorrhaging as my heart rate and blood pressure falsely appeared that I was hemodynamically stable. My stat CT was canceled and my OB and resident rushed me down the hallway themselves with my husband and I helped them find the nearest available OR. I was scheduled for a STAT emergency exploratory surgery (laparotomy) to look for the bleed, a clot, and had to sign papers for a hysterectomy if needed to save my life. A fuming anesthesiologist yelled at the nurse for trying to take my blood pressure as it was a life-threatening situation. He told my husband to prepare I may not make it and he couldn’t come but could wait in the NICU. When transferring me to the OR table I screamed in pain so loud I scared some of them! A handsome gentleman with blue eyes told me he’d take care of me and put me to sleep and with a quick mask, I was out.
I woke up choking and couldn’t breathe! I learned I was intubated and angrily comprehended I wasn’t suctioned after. I was told by the resident I had 5 units of blood transfusions with an estimated blood loss of 500ccs requiring 2 units of PRBCs and 2 units of FFP in OR with another unit in recovery. My c-section scar was reopened and, in my bladder’s peritoneum found a huge clot, a pelvic hematoma! They looked everywhere for the source of the bleed but my infection made it hard to find the source. They used a baby powder-like substance to protect the areas and stop the bleeding as stitching nothing is worse. My OB said in 35 years he had never done anything like it! In our fifth hospital room, I had an A-line, 3 IV’s, foley, and oxygen because I had to be intubated, and a handy dandy fourth round of antibiotics. After pushing my recovery nurse, who wasn’t my nurse, I learned I got to keep my uterus. Because I lost so much blood, I was also on an EKG monitor and therefore wasn’t allowed to go to the NICU to see my daughter. I wasn’t allowed to eat despite it being 48 hours because they wanted to keep a close eye on my stomach. I begged my RN for some jello anyway and some juice. It hurt terribly to urinate from the clot and I wanted to cry or scream when I did. In addition, it was extremely painful to get up and move. So, I was given Dilaudid PCA (later narco), and Motrin for pain, and simethicone for gas pain – which was the worst!
Then next morning June 11th I got my EKG monitor off, catheter out, and extra 2 IVs out. My daughter’s feeding tube was removed and was placed in her nose so they said I could start feeding her breastmilk. All was well until the next day on June 12th I woke up screaming at 3 am with shortness of breath, fever spike, and elevated blood pressure. They were worried about a PE (clot in the lung), infection, and pneumonia so I had STAT CT, X-Ray, EKG, and troponins drawn. I had to get up and move for imaging and it was very painful! I had small pleural effusions of fluid near my lungs but is normal from the intubation. I had to use a respirator hourly to prevent me from getting pneumonia which HURT! All my tests came back normal but I started shaking and got a fever again and was forced to rest. They believed it was due to hormones. I had diarrhea and was tested for C-Diff which was negative and was from all the antibiotics. At the same time, my daughter developed E-coli infection and developed sepsis. Her bilirubin was also high so she was treated for jaundice overnight and was taken off oxygen. I was finally able to pump more than a drop to take to her. My C-diff was negative and we were waiting for crossmatching test to start another transfusion because my hemoglobin dropped to a 6 again and I got to see her in the NICU while we waited.
I spent 10 days in the hospital and after discharge, the car ride was incredibly painful and I yelped the whole 30 minutes home for every bump despite my husband’s best efforts. Our daughter was a fighter and spent 46 days in the NICU before we could bring her home just shy of being 2 months old actual age. I had to advocate for her more than I would have liked catching heart murmurs, ongoing congestion, and anemia. The word spread from resident to nurse to nurse about our story and everyone knew who we were and our history. My daughter was labeled as being very strong and beating all odds and expectations. I did develop an infection of my incision around 6 weeks postpartum, but my OBs and surgeon came to see me in the NICU to evaluate me and after antibiotics, for 10 days I didn’t need surgery. It took a long time for me to walk or ride in the car without pain and through the whole NICU stay, I couldn’t drive. This forced me to rely on my husband on his work breaks to take me or my dad. Only one of us could be in the NICU at a time so it made it very hard. As first-time parents, we had to learn alone. I had to work out a special arrangement with the charge nurse to pump while he saw her then wait in the car. We were exhausted and nobody could help us or see her because of covid. My daughter and I are still doing physical therapy weekly and are getting stronger every day.
If there was one thing I would want poly mamas to know it would be to do your research. Know your risks and educate yourself on what to expect and what should be done for every outcome. Lastly, listen to your instincts and advocate for yourself. Do not let anybody ignore you. If I did, I wouldn’t be alive today.
Check the updates tab above to read more…
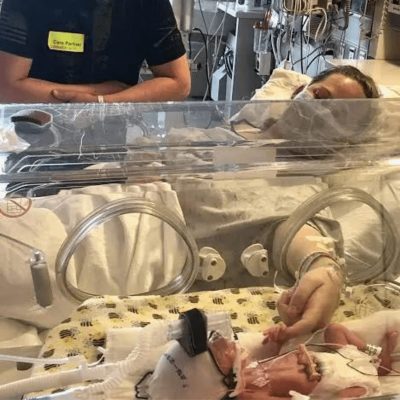

Jackilyn Hasn’t Written an Update Yet
But we do know from communicating with her that her sweet little girl was diagnosed at around 8 months old with DiGeorge Syndrome. Stay tuned as we hope to hear an update from Jackilyn soon!
